Photo Finish: Acute Dx: What Cause of Sudden Illness? rhus dermatitis
A 4-year-old girl presents with a highly pruritic rash. The day before, she had been playing outdoors at her grandmother's house. No pets were present, and the patient does not recall being stung or bitten by insects. There are bushes on the grandmother's property.
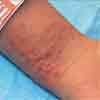
THE CASE:A 4-year-old girl presents with a highly pruritic rash. The day before, she had been playing outdoors at her grandmother's house. No pets were present, and the patient does not recall being stung or bitten by insects. There are bushes on the grandmother's property.
The next morning, a vesicular rash had erupted on the girl's wrists, posterior knees, and the corners of her mouth. Some of the vesicles ruptured after the patient scratched them. None of the other children with whom the patient was playing have similar symptoms. She has received the varicella vaccine and has a history of mild eczema.
The patient's vital signs are stable, and she is breathing and swallowing without difficulty. Oral examination reveals a small group of vesicles (0.1 to 0.2 cm) on the tip of her tongue (see Figure on page 738) and an erythematous dry, crusty rash in the corners of her mouth. There is no swelling in the mouth or throat. Vesicles on the wrists range from 0.25 cm to 0.5 cm and contain clear fluid. The 0.25-cm fluid-filled vesicles on the backs of the knees form a linear pattern. The patient has no stridor and the rest of the examination is unremarkable.
What is the most likely cause of this patient's symptoms?
Dyshidrotic eczema
Varicella
Impetigo
Rhus dermatitis (poison ivy)
(Answer and discussion on the next page.)
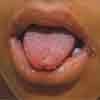
DISCUSSION: The patient had contracted rhus dermatitis after playing in a bush that was infested with poison ivy. Rhus dermatitismay be caused by poison ivy, poison sumac, or poison oak. The oil on the leaves, roots, and stems contain urushiols, highly allergenic compounds that cause a type IV hypersensitivity reaction. Allergic persons are sensitized to the compound before reacting to the oil. Our patient had had a previous case of poison ivy. Because this is a delayed hypersensitivity reaction, the vesicles appear 8 to 72 hours after contact.
Vesicle location depends on the site of exposure and whether the oil was transmitted along the skin by a vector, including scratching. Scratching creates a linear pattern. Lesions persist for 10 to 21 days. Vesicle fluid does not contain urushiol and does not cause further spread of the rash if the vesicle is ruptured. Clothing, tools, and other objects that are exposed to the oil must be washed because of the continued possibility of transmission.
Because the patient had no secondary infection, her treatment was symptomatic. Management included daily colloidal oatmeal baths, topical over-the-counter lotions, and cold, wet compresses followed by topical hydrocortisone 2.5% to relieve pruritus and swelling. The tongue vesicles were treated with topical anesthetics. In more severe cases, oral corticosteroids are taken daily and tapered over a 3-week period.
Dyshidrotic eczema (pompholyx) is a chronic relapsing and recurring eruption of vesicles on the palms, lateral fingers, and soles. The rash is highly pruritic and features symmetric vesicles that range from 0.1 to 0.5 cm. Although several causes have been proposed, the pathophysiology of dyshidrotic eczema is not yet understood. Sweat gland dysfunction was originally thought to be the principal cause, but this has been disputed.
Dyshidrotic eczema may be triggered by exogenous factors (such as infection or contact dermatitis), emotional stress, or environmental factors (for example, seasonal changes or humidity). Many patients have associated atopic dermatitis. The vesicles generally resolve in about 3 weeks. Treatment includes high- potency topical corticosteroids, oral corticosteroids, and antihistamines.
In patients with varicella, lesions at different stages--vesicles, pustules, and crusts--are present simultaneously. The 0.2- to 0.4-cm vesicles are described as "dew on a rose petal" because of the clear fluid and erythematous base. The disease is contagious as long as the vesicles are not all in the crust stage. Vesicles can form all over the body, including the oral cavity and vagina. Although our patient was vaccinated against varicella, the seroconversion rate after 1 dose is 95%. This leaves open the possibility of a less severe form called "breakthrough varicella." Treatment of varicella consists of antihistamines and mild antipruritic lotions.
Impetigo, which is most commonly caused by Staphylococcus aureus, has 2 clinical presentations--bullous and nonbullous. It typically appears on the face but can also involve the scalp, arms, and legs. Nonbullous impetigo usually has a honey-yellow crust that forms after the vesicles or pustules rupture. The erythematous base does not typically extend beyond the lesions.
The treatment for localized infections consists of topical antibiotic agents, such as mupirocin 2%. An oral antibiotic, such as cephalexin or dicloxacillin, is recommended for systemic disease.
References:
FOR MORE INFORMATION:
m Brodell RT, Williams L. Taking the itch out of poison ivy. Are you prescribing the right medication?
Postgrad Med.
1999;106:69-70.m Crosti C, Lodi A. Pompholyx: a still unresolved kind of eczema.
Dermatology.
1993;186:241-242.m Hirschmann JV. Impetigo: etiology and therapy.
Curr Clin Top Infect Dis.
2002;22:42-51.m Kunkel DB, Spoerke DG. Evaluating exposures to plants.
Emerg Med Clin North Am.
1984;2:133-144.m Wilkinson JD. Vesicular palmoplantar eczema. In: Freedburg IM, Eisen AZ, Wolff K, eds.
Fitzpatrick's Dermatology in General Medicine.
5th ed. New York: McGraw-Hill; 1999:1489-1494.
Recognize & Refer: Hemangiomas in pediatrics
July 17th 2019Contemporary Pediatrics sits down exclusively with Sheila Fallon Friedlander, MD, a professor dermatology and pediatrics, to discuss the one key condition for which she believes community pediatricians should be especially aware-hemangiomas.