More than stubborn diaper rash?
An 11-month-old boy was brought to the doctor by anxious parents for the evaluation of persistent diaper dermatitis. Despite trying multiple barrier creams and over-the-counter antifungal products, the rash did not resolve.
Figure
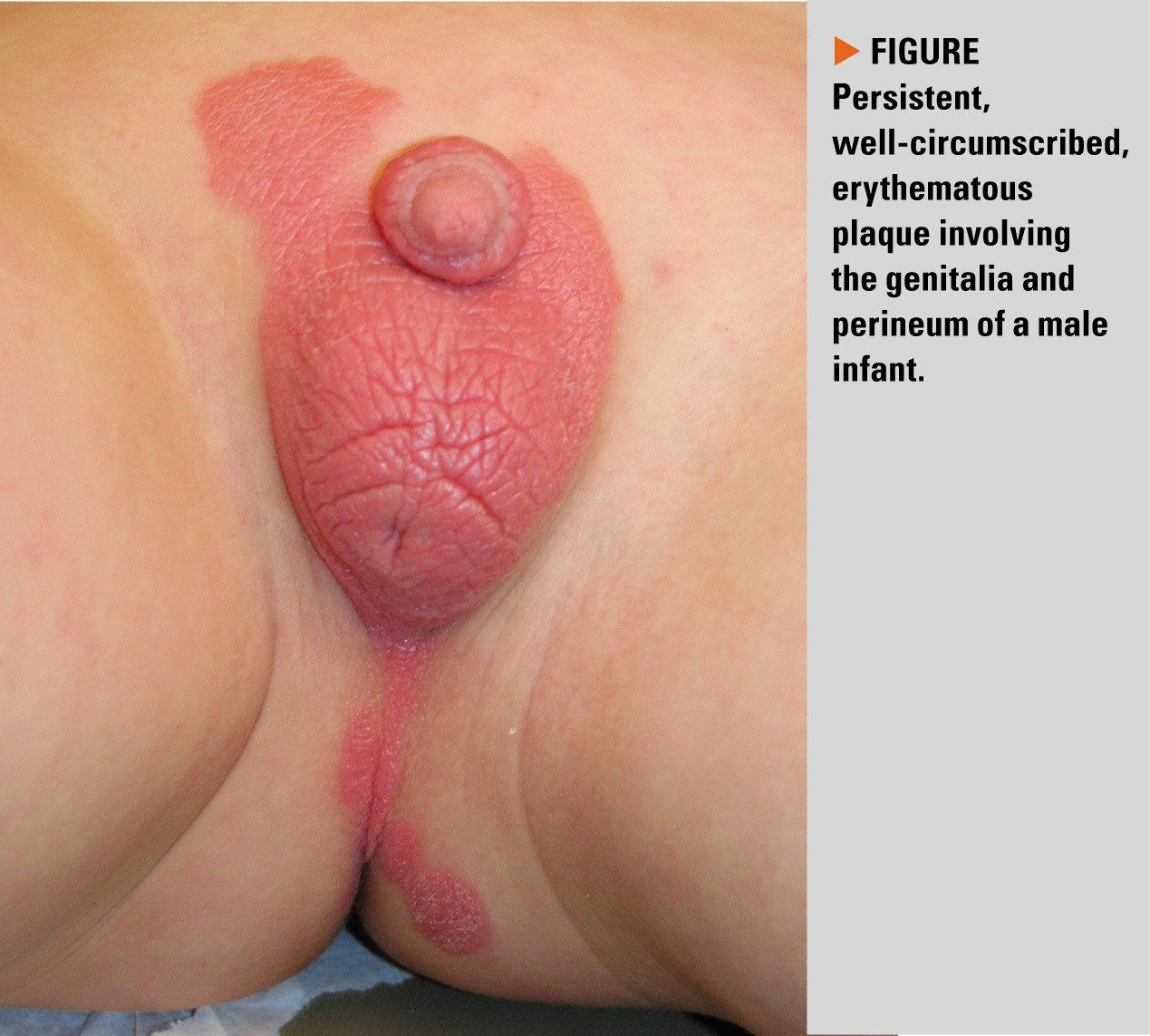
The case
An 11-month-old boy was brought to the doctor by anxious parents for the evaluation of persistent diaper dermatitis. Despite trying multiple barrier creams and over-the-counter antifungal products, the rash did not resolve.
Infantile psoriasis
Etiology and epidemiology
Psoriasis is a chronic inflammatory condition that has a prevalence of approximately 1% in children.1 Of those who develop psoriasis, up to 30% start with psoriasis in the diaper area, also known as napkin psoriasis, within the first 2 years of life.2 Infantile psoriasis is more commonly preceded by an infection or trauma than in adult psoriasis, and the Koebner phenomenon from repeated wiping and rubbing on a diaper is a likely culprit for napkin psoriasis.3 Family history of psoriasis is also a risk factor for developing this entity, and those who have dissemination of psoriatic plaques beyond the diaper area are at a higher risk of having psoriasis later in life.4
Clinical findings
Infantile psoriasis typically presents as a persistent, well-demarcated red plaque with absent or scant scale distributed in the diaper area. The plaques can involve the skinfolds. Some infants may have psoriatic plaques elsewhere on the body, but the groin involvement often precedes the more widespread eruption. Some infants exclusively have involvement of the diaper area.5
Differential diagnosis
Infantile psoriasis is often confused with irritant contact dermatitis, allergic contact dermatitis, seborrheic dermatitis, or candidiasis.
Irritant contact dermatitis is the most common cause of diaper dermatitis, and it results from wet, soiled diapers rubbing against the skin. This only affects the areas of skin exposed to the diaper, and it often affects the prominent skin most in contact with the diaper while sparing the skin folds.6
Allergic contact dermatitis may occur after using a product that contains an ingredient to which the infant is sensitized. This outbreak may involve skin beyond the confines of the diaper area, and it will subside 2-4 weeks after the discontinuation of the culprit product.6
Seborrheic dermatitis presents as erythematous, well-demarcated patches in the diaper area, but it is often erythematous with an overlying greasy scale when present in the scalp, face, ears, and neck. Erythematous plaques may also be present in intertriginous areas in infants, including in the skin folds on legs and arms.6
Candidiasis presents as a bright red eruption that starts in the inguinal folds and may involve the entire diaper area. Erythematous or pustular satellite lesions may be scattered around the periphery of the involved areas.7
Management
Infantile psoriasis is characteristically resistant to standard diaper dermatitis treatments. Topical therapies, including low potency topical steroid ointments and barrier creams often provide temporary control, but lesions often return. Short courses of mid- or high-potency steroids can be used for recalcitrant lesions if necessary. Topical calcineurin inhibitors such as tacrolimus and pimecrolimus can also be used safely and effectively in the diaper area.5
Patient outcome
The patient was prescribed hydrocortisone 2.5% ointment to apply twice daily for up to 2 weeks, and tacrolimus 0.03% ointment to apply thereafter. His parents were counseled to use a barrier cream during every diaper change.
References:
1. Tollefson MM, Crowson CS, McEvoy MT, et al. Incidence of psoriasis in children: a population based study. J Am Acad Dermatol 2010;62(6):979–87.
2. Morris A, Rogers M, Fischer G, et al. Childhood psoriasis: a clinical review of 1262 cases. Pediatr Dermatol 2001;18(3):188–98.
3. Ozden MG, Tekin NS, Gürer MA, Akdemir D, Doçramacñ C, Utas S, et al: Environmental risk factors in pediatric psoriasis: a multicenter case-control study. Pediatr Dermatol 2011;28:306–312.
4. Benoit S, Hamm H. Childhood psoriasis. Clin Dermatol 2007;25(6):555–62.
5. Cohen BA. “Neonatal Dermatology.” Pediatric Dermatology, 4th ed., Elsevier Saunders, 2013, pp. 14–67.
6. Cohen B. Differential Diagnosis of Diaper Dermatitis. Clin Pediatr. 2017; 56(5S):16S-22S.
7. Morrell DS, Cathcart SD, Carder KR. “Fungal Infections, Infestations, and Parasitic Infections in Neonates and Infants.” Neonatal and Infant Dermatology, 3rd ed., Elsevier Saunders, 2015, pp. 198-215.

Recognize & Refer: Hemangiomas in pediatrics
July 17th 2019Contemporary Pediatrics sits down exclusively with Sheila Fallon Friedlander, MD, a professor dermatology and pediatrics, to discuss the one key condition for which she believes community pediatricians should be especially aware-hemangiomas.