Photo Essay: Fixed Drug Eruption
An 8-year-old boy was brought to the emergency department with fever, bloody and mucous diarrhea, and abdominal pain. Specimens for stool culture were sent to the laboratory, and therapy with trimethoprim/sulfamethoxazole (TMP/SMX) was initiated.
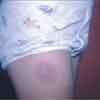
An 8-year-old boy was brought to the emergency department with fever, bloody and mucous diarrhea, and abdominal pain. Specimens for stool culture were sent to the laboratory, and therapy with trimethoprim/sulfamethoxazole (TMP/SMX) was initiated. Hours after the first dose was given, the child complained of itching on the lateral aspect of the right thigh. Within the next 2 days, a well-defined, erythematous lesion with a central blister developed. The patient's mother remembered that 2 years earlier, a similar lesion had developed in the same area after the child was given TMP/SMX for a urinary tract infection.
This lesion is characteristic of a fixed drug eruption--an unusual reaction in which a lesion recurs in the same area when the patient is rechallenged by the offending drug. Sulfon- amides, antibiotics, anticonvulsants, analgesics, and anti-inflammatory drugs are most commonly associated with fixed drug eruptions.1,2
The reaction usually develops within hours of taking the drug. After the first exposure, a solitary lesion may appear. After re-exposure to the same drug, new lesions may arise and the recurrent lesion may be larger than the original.3 The most commonly affected areas are the hands, feet, and genitalia; the limbs are more frequently affected than the trunk. Perioral and periorbital lesions may occur. Patients may have mild localized pruritus; systemic symptoms, such as fever, are absent or mild.
A fixed drug eruption may worsen for a few days after the responsible agent is discontinued and then resolve slowly over 1 or more weeks. As the lesion heals, crusting and scaling develop, leaving a persistent, dusky brown discoloration. The hyperpigmentation--which may be more pronounced in persons with brown skin--usually fades over time.
Within 10 days after TMP/SMX was discontinued, this child's lesion resolved, leaving a brownish pigmentation. The child's fever, abdominal pain, and diarrhea were attributed to bacterial gastroenteritis caused by TMP/SMX-resistant Shigella flexneri. He responded quickly to treatment with ciprofloxacin.
(Case and photographs courtesy of Elias Milgram, MD, of Miami.)
References:
REFERENCES:
1.
Daoud MS, Schanbacher CF, Dicken CH. Recognizing cutaneous drug eruptions. Reaction patterns provide clues to causes.
Postgrad Med.
1998;104:101-104, 107-108, 114-115.
2.
Stern RS, Wintroub BU. Cutaneous reactions to drugs. In: Freedberg IM, Eisen AZ, Wolff K, et al, eds.
Fitzpatrick's Dermatology in General Medicine.
6th ed. New York: McGraw-Hill; 2003:1633-1642.
3. Hurwitz S. Clinical Pediatric Dermatology. 2nd ed. Philadelphia: WB Saunders; 1993:67-68.
Recognize & Refer: Hemangiomas in pediatrics
July 17th 2019Contemporary Pediatrics sits down exclusively with Sheila Fallon Friedlander, MD, a professor dermatology and pediatrics, to discuss the one key condition for which she believes community pediatricians should be especially aware-hemangiomas.